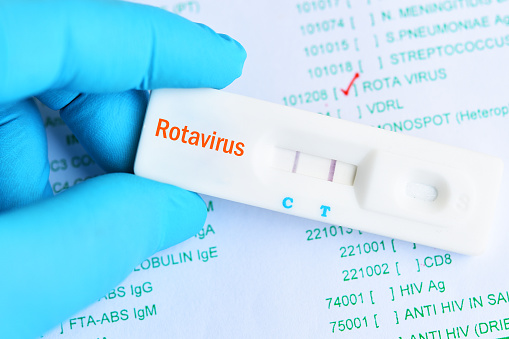
Rotavirus is an important pathogen that causes severe diarrhea in infants aged 6 months to 2 years old. It has strong seasonality and mostly occurs in autumn and winter. Diarrhea in infants and young children caused by rotavirus is mainly transmitted by the fecal-oral route. In the early stage of the disease, the children manifested as cold symptoms such as runny nose, cough, fever, and sore throat. 20 times. If the treatment is not timely or the treatment method is incorrect, children are prone to life-threatening dehydration, pneumonia and toxic myocarditis. There are 111 to 135 million cases of diarrhea caused by rotavirus infection globally each year, resulting in 600,000 infant deaths. Therefore, early detection, early diagnosis, and early treatment are the keys to reducing the mortality and complications of rotavirus infection.
Rotavirus is one of the major causes of acute diarrhea in humans and animals worldwide. According to the antigenicity of rotavirus, it is currently divided into A~G7 groups, among which group A rotavirus is the main pathogen of infantile diarrhea in autumn and winter. In developing countries, nearly one million children die each year from rotavirus infection, which is mainly related to environmental sanitation, nutritional status and other factors. Group B rotavirus mainly infects young adults; group C rotavirus mainly infects young people, causing sporadic epidemics. The infection rate of rotavirus was 89.4% before the age of 36 months, and severe rotavirus infection was mainly seen in infants aged 6-24 months. Because infants younger than 6 months have immunity from the mother and milk contains a large amount of SIgA, which provides immune protection, therefore, the infection rate of rotavirus is low; After rotavirus infection, the level of specific anti-rotavirus antibodies in serum and intestinal secretions increases, which can prevent rotavirus infection and reduce the infection rate. Therefore, rapid and accurate laboratory diagnosis of rotavirus is of great significance for the prevention and control of rotavirus diarrhea.
The virus spreads from person to person, especially when people with diarrhea do not wash their hands thoroughly after defecation. People can also get infected if they touch their mouth after touching fecal items that contain an infection, such as toys and diapers. All such transmissions involving infected feces are referred to as fecal-oral transmission. People get the virus if they eat or drink food or water that has been contaminated with the virus. Adults can also become infected after close contact with infected children, but are less likely to develop serious illness.
In winter, rotavirus is the most common cause of diarrhea, and infants and young children can be seriously ill and require hospital treatment.
Typical symptoms
During rotavirus infection, vomiting usually lasts for 2 to 6 days, and diarrhea lasts for 1 to 9 days, with an average of 5 days; the peak of rotavirus excretion in stool is 3 days before the course of the disease, and 68% of patients usually have fever symptoms. Therefore, watery or egg-like soup-like stools and a high incidence of vomiting, especially vomiting that often occurs before diarrhea, are the prominent symptoms of rotavirus diarrhea in children. Rotavirus diarrhea occurs all over the world. In tropical regions, the disease can occur throughout the year without obvious seasonality. Occasionally, there are epidemic outbreaks of the disease in dry seasons; in temperate countries, its incidence has obvious seasonality. .
Route of infection
Like most enteroviruses, it is mainly transmitted by the fecal-oral route, and "diseases enter from the mouth", that is, ingestion of food and water contaminated with rotavirus. In addition, eating and aerosols in the air after touching contaminated items with hands also have the possibility of transmission.
The immunocolloidal gold method can accurately, quickly and easily determine the rotavirus antigen, which plays a very important role in identifying the pathogen, controlling the spread, formulating effective treatment measures, and preventing the abuse of antibiotics. To provide a basis for clinical treatment, help to reduce complications, thereby reducing the mortality rate.